Medication costs make up over 10% of health care dollars and are the fastest growing source of medical expense. Many state and federal officials have called for action that 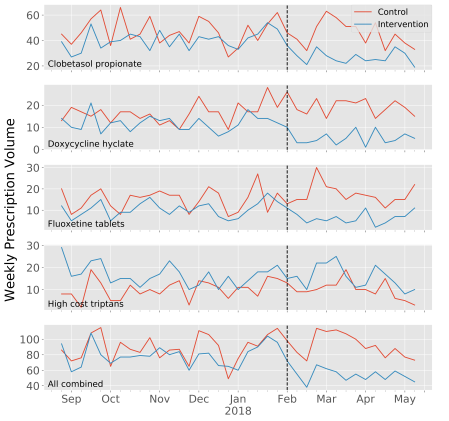 would add cost transparency to the complex, opaque medication supply chain believing that this will lead to lower prices and higher value care. Though this may appeal to our intuition, evidence that medication cost transparency leads to higher value care is scant. In order to add to the evidence base, four other investigators and I embarked on a 9-month investigation designing and evaluating the effect of medication cost transparency decision support built into the electronic health record. Bottom line: it makes a difference. The results were recently published and are available on the JAMIA website: https://academic.oup.com/jamia/advance-article-abstract/doi/10.1093/jamia/ocz025/5445905.
would add cost transparency to the complex, opaque medication supply chain believing that this will lead to lower prices and higher value care. Though this may appeal to our intuition, evidence that medication cost transparency leads to higher value care is scant. In order to add to the evidence base, four other investigators and I embarked on a 9-month investigation designing and evaluating the effect of medication cost transparency decision support built into the electronic health record. Bottom line: it makes a difference. The results were recently published and are available on the JAMIA website: https://academic.oup.com/jamia/advance-article-abstract/doi/10.1093/jamia/ocz025/5445905.
research
Why the stakes are so high in the open data debate
It is hard to understate just how much of a currency data has become in medicine. Whether talking about evidence-based medicine, precision medicine, or genomics, the ability to collect and distill data into information, transform it into knowledge, and use that knowledge to drive effective action is at the heart of what modern medicine seeks to accomplish. The centrality of data to this process has created well-entrenched stakeholders, which is why it comes as no surprise that the conversation around open sharing of research data following publication has shifted into controversial territory.
On the Evaluation of symptom checkers for self diagnosis and triage: audit study
I should begin by acknowledging the authors’ important contribution to elucidating the gap between what symptom checkers may hope to provide and the existing state of the art. Semigren et al adopt a pragmatic approach both by identifying which symptom checkers patients may reasonably find and assessing them in the most intuitive way imaginable: making them take the standardized patient tests we all take in medical school.
How Motor Learning Generalizes
Introduction
Every movement we make requires our brains to predict what forces–gravity, an object we’re holding, a strong gust of wind–each of our body  parts will experience in order to move in a coordinated fashion. No movement is ever exactly the same and so it is remarkable that we are not constantly tripping over ourselves. It is well-known that humans learn based on previous errors in their movements. My work at the Harvard Neuromotor Control Lab was to investigate how the brain learns to “makes generalizations” about movements and learn from its mistakes. Continue reading
parts will experience in order to move in a coordinated fashion. No movement is ever exactly the same and so it is remarkable that we are not constantly tripping over ourselves. It is well-known that humans learn based on previous errors in their movements. My work at the Harvard Neuromotor Control Lab was to investigate how the brain learns to “makes generalizations” about movements and learn from its mistakes. Continue reading
Understanding Tracheostomy as a Risk Factor for Sternal Wound Infections
Introduction
Tracheostomy is an unpleasant, but effective means for transitioning patients off ventilatory support after prolonged periods of respiratory failure following cardiac surgery. There is, however, a perceived risk of patients getting infections of the surgical, sternal  wound if tracheostomy is performed too early. This perceived risk means patients are often delayed in tracheostomy, including the benefits of ability to speak, reduced mortality, reduced ICU stay, and reduced delirium until the surgical wound is felt no longer at risk. Continue reading
wound if tracheostomy is performed too early. This perceived risk means patients are often delayed in tracheostomy, including the benefits of ability to speak, reduced mortality, reduced ICU stay, and reduced delirium until the surgical wound is felt no longer at risk. Continue reading